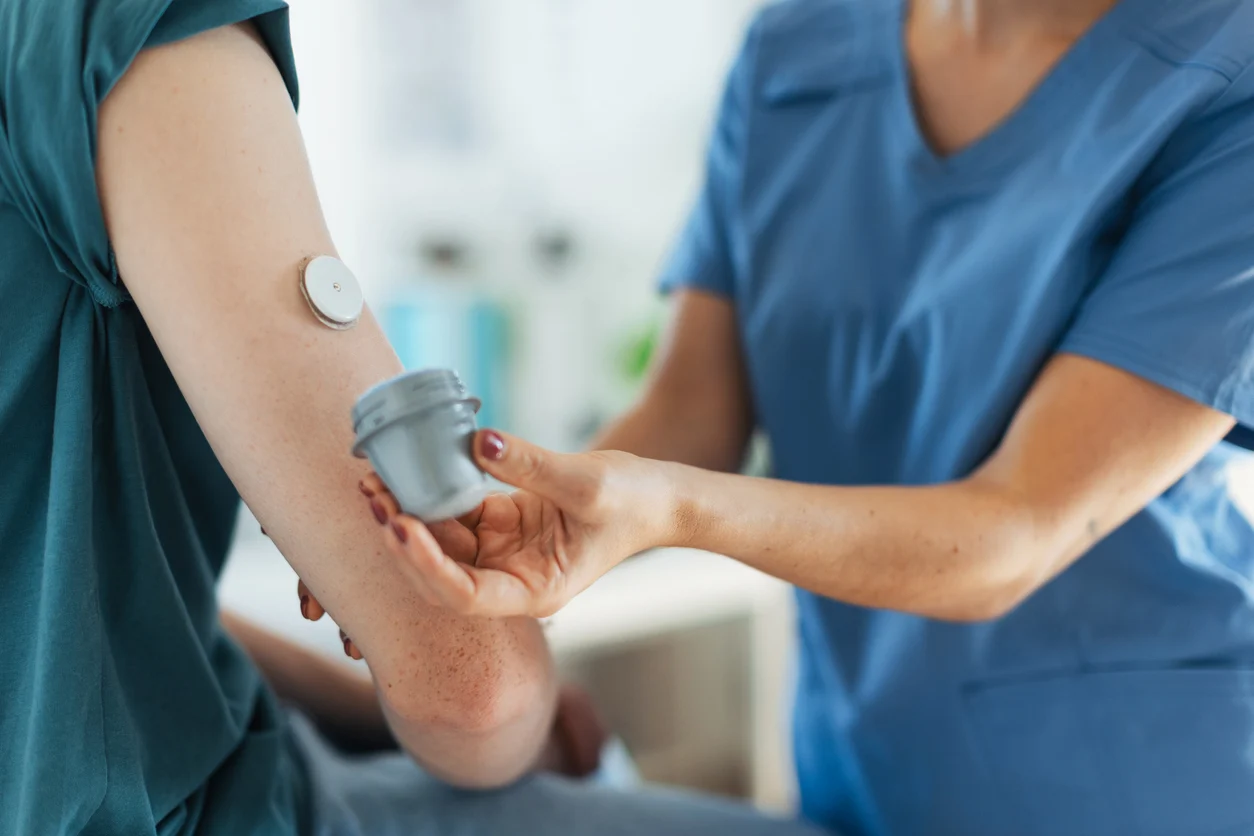
Skin reactions to glucose sensors (like continuous glucose monitors, or CGMs) are fairly common in children, especially those with sensitive skin or a history of eczema.
These reactions are usually caused by adhesives, friction, moisture buildup, or allergic responses (often to acrylates used in sensor adhesives). Here’s a practical, evidence-informed overview of prevention and treatment strategies.
Common Types of Skin Reactions
Irritant contact dermatitis: Redness, dryness, mild peeling
Allergic contact dermatitis: Itching, swelling, blisters (delayed reaction)
Pressure/friction injury: Soreness or broken skin
Infection (rare): Warmth, pus, increasing pain
Prevention Strategies
1. Skin Preparation
Clean with mild soap and water; avoid alcohol if skin is sensitive
Ensure the skin is completely dry before applying the sensor
Avoid applying to recently shaved or damaged skin
2. Barrier Methods
Apply a barrier film (e.g., Cavilon or Skin Prep wipes) before sensor placement
Use a hydrocolloid dressing or thin silicone layer under the sensor (cut a hole for the filament if needed)
Consider hypoallergenic adhesive patches (e.g., Tegaderm, IV3000) beneath or over the sensor
3. Rotation of Sites
Rotate insertion sites regularly (abdomen, upper buttocks, back of arms depending on device guidelines)
Avoid reusing irritated areas until fully healed
4. Device-Specific Adjustments
Some devices (like Dexcom G6 or FreeStyle Libre) have known adhesive sensitivities—trial different placements or protective layers
Contact manufacturers for alternative adhesives or samples
5. Sweat & Moisture Control
Apply sensors to less sweaty areas
Use additional adhesive overlays if peeling occurs
Treatment Strategies
1. Mild Reactions
Remove the sensor if irritation worsens
Apply emollients (fragrance-free moisturizers)
Use a short course of low-potency topical corticosteroids (e.g., hydrocortisone) after sensor removal
2. Moderate to Severe Reactions
Topical corticosteroids (prescribed strength if needed)
Oral antihistamines for itching
Consider referral to a dermatologist for patch testing (to confirm acrylate allergy)
3. Suspected Infection
Look for spreading redness, warmth, discharge
Seek medical care—may require topical or oral antibiotics
When to Seek Specialist Help
Recurrent or worsening reactions despite prevention
Blistering or ulceration
Suspected allergic contact dermatitis (especially to adhesives)
Practical Tips for Parents
Keep a skin diary to track reactions and triggers
Take photos to monitor progression
Work with your diabetes care team to balance glucose monitoring needs with skin health
Emerging Solutions
Newer CGM adhesives designed for sensitive skin
Custom barrier patches and “sandwich” layering techniques
Research into acrylate-free adhesives is ongoing
Advanced & Emerging Approaches
6. Patch Testing & Allergen Identification
If reactions persist, a dermatologist can perform patch testing to identify specific allergens (commonly isobornyl acrylate).
Knowing the exact trigger helps tailor prevention—for example, choosing barriers that block that allergen effectively.
7. “Sandwich Technique” (Layered Protection)
This is widely used in pediatric diabetes care for children with recurrent reactions:
Apply barrier film
Place a thin hydrocolloid or silicone dressing
Insert the sensor through a small cut hole
Secure with an overpatch
This reduces direct adhesive-skin contact while maintaining sensor accuracy.
8. Desensitization & Skin Conditioning
In some cases:
Gradual exposure to adhesives (short wear times initially)
Regular use of moisturizers to strengthen the skin barrier
Avoid over-cleansing, which can weaken the skin
9. Alternative Devices or Wearing Strategies
Some children tolerate one system better than another:
Dexcom G7 may have different adhesive composition compared to FreeStyle Libre 2
Shorter wear cycles or planned “skin rest days” can reduce cumulative irritation
Age-Specific Considerations
Infants & Toddlers
Skin is thinner and more permeable → higher irritation risk
Prefer gentle barriers and minimal adhesive layers
Frequent site checks by caregivers
School-Age Children
Increased sweating and activity
Reinforce secure placement and protective overlays
Adolescents
Hormonal changes may increase oil/sweat
Encourage self-monitoring of skin and early reporting of irritation
Balancing Skin Health with Glucose Control
Continuous glucose monitoring is essential for managing Type 1 Diabetes, so the goal is not to stop CGM use but to adapt the interface between device and skin.
A practical approach:
Mild irritation → adjust barrier strategy
Recurrent irritation → rotate sites + try different materials
Severe allergy → dermatology referral + consider alternative systems
Recommended Skincare Routine Around Sensor Use
Before application:
Clean → dry → barrier film (if needed)
During wear:
Avoid scratching
Keep area dry
Reinforce edges if peeling
After removal:
Clean gently
Apply moisturizer
Use topical steroid only if inflamed (short-term)
What to Avoid
Applying sensors on broken or inflamed skin
Using harsh removers repeatedly (can worsen irritation)
Ignoring early signs of allergy (they tend to worsen over time)
Future Directions
Acrylate-free adhesives
Breathable, skin-mimicking sensor interfaces
Non-invasive glucose monitoring technologies (under development)
Clinical Algorithm (Stepwise Approach)
Step 1: Identify the reaction
Mild redness/itch → likely irritant dermatitis
Itchy rash with delayed onset → suspect allergic dermatitis
Pain, warmth, discharge → rule out infection
Step 2: Immediate action
Mild → continue CGM with added barrier protection
Moderate → remove sensor, treat skin, reapply at new site with protection
Severe → stop use temporarily and seek medical evaluation
Step 3: Prevent recurrence
Introduce barrier film or dressing
Change insertion site
Trial a different device (e.g., Dexcom G6 vs FreeStyle Libre 3)
Step 4: Escalate if needed
Dermatology referral
Patch testing for allergens
Consider long-term skin protection strategies
Guidance for Healthcare Providers
Take complaints seriously early: mild irritation can evolve into chronic dermatitis
Document reactions: include photos and timing relative to sensor application
Educate families: demonstrate barrier techniques in clinic
Prescribe appropriately:
Low- to mid-potency topical corticosteroids
Non-steroidal anti-inflammatory creams (e.g., calcineurin inhibitors if recurrent)
Coordinate care between endocrinology and dermatology
Parent-Friendly Action Plan
If you notice redness:
Don’t panic—remove the sensor if worsening
Clean gently and let the skin rest
Apply moisturizer
If itching or rash appears repeatedly:
Try a barrier layer next time
Switch site and monitor closely
If severe symptoms appear (blisters, swelling):
Stop using that site
Contact your healthcare provider
Practical “Real-Life” Tips
Apply sensors in the evening so adhesives settle overnight
Warm the adhesive slightly with your hands before applying (improves sticking, may reduce irritation from movement)
Use adhesive remover sprays gently to avoid skin stripping
Trim, don’t shave, hair in the area to reduce microtrauma
Research Insights (Simplified)
A significant proportion of pediatric CGM users experience some form of skin reaction
Acrylate allergy is one of the most common confirmed causes in persistent cases
Barrier methods significantly reduce incidence when used consistently
No single strategy works for all—individualization is key
Key Takeaways
Skin reactions are common but manageable
Early prevention is more effective than treatment
Barrier techniques and site rotation are the cornerstone
Persistent cases need specialist input
The goal is to maintain continuous glucose monitoring safely, especially in children with Type 1 Diabetes
Skin Sensitivity to Glucose Sensors in Children: Prevention and Treatment Strategies (Extended Review)
Introduction
The use of continuous glucose monitoring (CGM) systems has transformed the management of Type 1 Diabetes in children. Devices such as Dexcom G6, Dexcom G7, and FreeStyle Libre 3 provide real-time glucose data, improve glycemic control, and reduce the burden of frequent fingerstick testing. However, alongside these benefits, dermatological complications—particularly skin sensitivity and irritation at sensor sites—have emerged as a significant clinical challenge, especially in pediatric populations.
Children are uniquely vulnerable due to thinner skin, increased transepidermal water loss, higher activity levels, and a greater likelihood of atopic conditions such as eczema. This article provides a comprehensive overview of the mechanisms, risk factors, prevention strategies, and treatment approaches for skin reactions associated with CGM use in children.
Pathophysiology of Skin Reactions
Skin reactions to CGM systems are generally categorized into three main types:
1. Irritant Contact Dermatitis (ICD)
This is the most common reaction and results from:
Mechanical friction from the device
Occlusion and moisture buildup under adhesives
Repeated application and removal of adhesive materials
ICD typically presents as mild erythema, dryness, or scaling and is usually localized to the adhesive area.
2. Allergic Contact Dermatitis (ACD)
ACD is an immune-mediated delayed hypersensitivity reaction. A key allergen implicated in CGM-related ACD is isobornyl acrylate (IBOA), a component found in some adhesives.
Clinical features include:
Intense itching
Erythema extending beyond the adhesive border
Vesicles or blistering in severe cases
Unlike irritant reactions, ACD tends to worsen with repeated exposure.
3. Secondary Complications
Skin infections (bacterial or fungal)
Post-inflammatory hyperpigmentation
Skin barrier disruption, increasing susceptibility to future irritation
Risk Factors in Children
Several factors increase the likelihood of skin sensitivity in pediatric CGM users:
History of atopic dermatitis (eczema)
Younger age (immature skin barrier)
Frequent sensor changes
Excessive sweating (common in active children)
Improper removal techniques causing skin trauma
Genetic predisposition to contact allergies
Prevention Strategies
Effective prevention requires a proactive, individualized approach.
Skin Preparation
Proper preparation reduces irritation risk:
Clean the skin with mild, fragrance-free cleansers
Avoid alcohol-based products in sensitive individuals
Ensure the skin is completely dry before application
Barrier Protection Techniques
Barrier methods are the cornerstone of prevention:
Barrier Films
Thin polymer layers (e.g., Cavilon) applied before sensor placement:
Reduce direct contact between adhesive and skin
Allow adhesion while protecting the epidermis
Hydrocolloid or Silicone Dressings
Provide a physical buffer layer
Particularly useful in children with known adhesive sensitivity
The “Sandwich Technique”
A widely used method in pediatric care:
Apply barrier film
Add a hydrocolloid dressing
Insert sensor through a small opening
Secure with an overlay patch
This technique minimizes allergen exposure without compromising device function.
Site Rotation
Rotating sensor placement is essential:
Prevents cumulative skin damage
Allows healing time between applications
Common sites include abdomen, upper buttocks, and posterior arms
Moisture and Sweat Management
Choose less sweaty areas for placement
Use breathable adhesive patches
Reinforce edges with overpatches when needed
Device Selection
Different CGM systems use different adhesive formulations. Some children may tolerate one device better than another:
Dexcom G7 may differ in adhesive composition compared to FreeStyle Libre 2
Trial and error is sometimes necessary
Treatment Strategies
Management of Mild Reactions
Continue CGM use with added barrier protection
Apply fragrance-free emollients after sensor removal
Monitor closely for progression
Management of Moderate Reactions
Remove the device temporarily
Apply low-potency topical corticosteroids (e.g., hydrocortisone)
Resume CGM with enhanced protective strategies
Management of Severe Reactions
Discontinue sensor use until healing occurs
Use prescription-strength topical corticosteroids
Consider oral antihistamines for itching
Refer to dermatology for further evaluation
Allergic Contact Dermatitis Management
Patch testing to identify allergens
Strict avoidance of identified substances
Use of alternative barrier materials or devices
Infection Management
Signs include:
Increasing redness
Warmth
Pus or discharge
Treatment may involve:
Topical antibiotics
Oral antibiotics in more severe cases
Psychosocial Impact
Skin complications can significantly affect:
Adherence to CGM use
Quality of life
Parental anxiety
Children may resist wearing devices due to discomfort or cosmetic concerns. Addressing skin issues promptly is essential to maintain long-term adherence and optimal diabetes control.
Clinical Considerations for Healthcare Providers
Early identification and intervention are critical
Educate families on preventive techniques
Encourage routine skin assessment
Collaborate with dermatologists for complex cases
Future Directions
Emerging innovations aim to reduce dermatological complications:
Acrylate-free adhesives
Biocompatible, breathable materials
Non-invasive glucose monitoring technologies (under development)
Ongoing research continues to focus on improving both device performance and skin compatibility.
Conclusion
Skin sensitivity to CGM devices in children is a common but manageable issue. With proper prevention strategies, early recognition, and individualized care, most children can continue to benefit from continuous glucose monitoring without significant disruption.
Maintaining a balance between effective glucose control and skin health is essential. Through collaboration between families, healthcare providers, and device manufacturers, outcomes can be optimized for pediatric patients living with Type 1 Diabetes.