Introduction: The Burden of Injections in Pediatric Diabetes
For children with type 1 diabetes, daily insulin injections are a painful and anxiety-inducing necessity. The fear of needles can lead to poor adherence, impacting glycemic control and increasing the risk of complications.
This challenge has spurred global research into non-invasive insulin delivery methods that could transform diabetes management for young patients.
Global Innovations in Needle-Free Insulin Delivery
1. Transdermal Delivery Systems
Recent advancements have focused on delivering insulin through the skin without needles. A notable development is the powder needleless injection (PNI) device, which uses high-speed gas to deliver insulin powder transdermally.
Studies have demonstrated its efficacy in animal models, suggesting potential for human application .
2. Microneedle Patches
Microneedle technology employs tiny, painless needles to deliver insulin through the skin. These patches can provide controlled insulin release, improving glycemic control without the discomfort of traditional injections.
Research is ongoing to optimize their design and efficacy for pediatric use .
3. Inhalable Insulin
Inhalable insulin offers a non-invasive alternative by delivering insulin through the lungs. While adult formulations exist, adapting this technology for children requires careful consideration of dosing and lung development.
Clinical trials are underway to assess its safety and effectiveness in pediatric populations .
Challenges and Considerations
Despite promising developments, several challenges remain:
Bioavailability: Ensuring consistent and adequate insulin absorption through non-invasive methods is critical.
Long-Term Safety: The long-term effects of new delivery systems, especially in children, need thorough evaluation.
Regulatory Approval: Gaining approval from health authorities requires extensive clinical data demonstrating safety and efficacy.
Cost and Accessibility: Making these technologies affordable and accessible globally is essential to benefit all children with diabetes.
The Road Ahead
The pursuit of needle-free insulin delivery for children is gaining momentum worldwide. Collaborative efforts among researchers, clinicians, and industry stakeholders are crucial to overcome existing barriers.
With continued innovation and rigorous testing, these technologies hold the promise of transforming diabetes care, making it less invasive and more child-friendly.
Is the Treatment of Children’s Diabetes Without Injections on the Way? — Continued
More Global Projects and Emerging Technologies
Beyond the approaches already discussed, several major research initiatives and innovative companies around the world are actively working toward needle-free or minimally invasive diabetes treatment for children.
4. Oral Insulin (Insulin Pills or Capsules)
One of the most ambitious goals in diabetes research is to develop oral insulin, similar to a pill, so that children could swallow insulin instead of injecting it.
Why is this difficult?
Insulin is a protein, and proteins are usually broken down by stomach acid and digestive enzymes before they can enter the bloodstream. This has made oral insulin extremely challenging.
Current global efforts:
India (Biocon and partners):
Researchers have developed an oral insulin formulation that protects insulin as it passes through the stomach and releases it in the intestine. Early clinical studies in adults have shown promising glucose-lowering effects, and pediatric research may follow.
USA and Europe (various biotech firms):
Several companies are using nanoparticle technology to “package” insulin inside protective carriers that can survive digestion and deliver insulin into the bloodstream.
Potential impact for children:
If successful, oral insulin could:
Eliminate injections completely
Reduce fear and anxiety
Improve treatment adherence
Make diabetes management feel more “normal” for children
However, this technology is still in experimental stages and likely several years away from routine use.
5. Smart Insulin (Glucose-Responsive Insulin)
This is one of the most exciting and futuristic concepts in diabetes treatment.
What is smart insulin?
Smart insulin is designed to turn on when blood sugar is high and turn off when blood sugar is normal or low—similar to how a healthy pancreas works.
Global research:
United States (MIT, Harvard, and other institutions):
Scientists are developing insulin that binds to glucose-sensitive molecules. When glucose levels rise, the insulin becomes active; when glucose levels fall, it becomes inactive.
Europe (UK and Germany collaborations):
Research groups are testing smart insulin in animal models with encouraging results.
What this could mean for children:
One or two injections per day instead of multiple
Greatly reduced risk of hypoglycemia
Less need for constant monitoring and adjustment
While not completely “needle-free,” this would dramatically reduce injections and complexity of care.
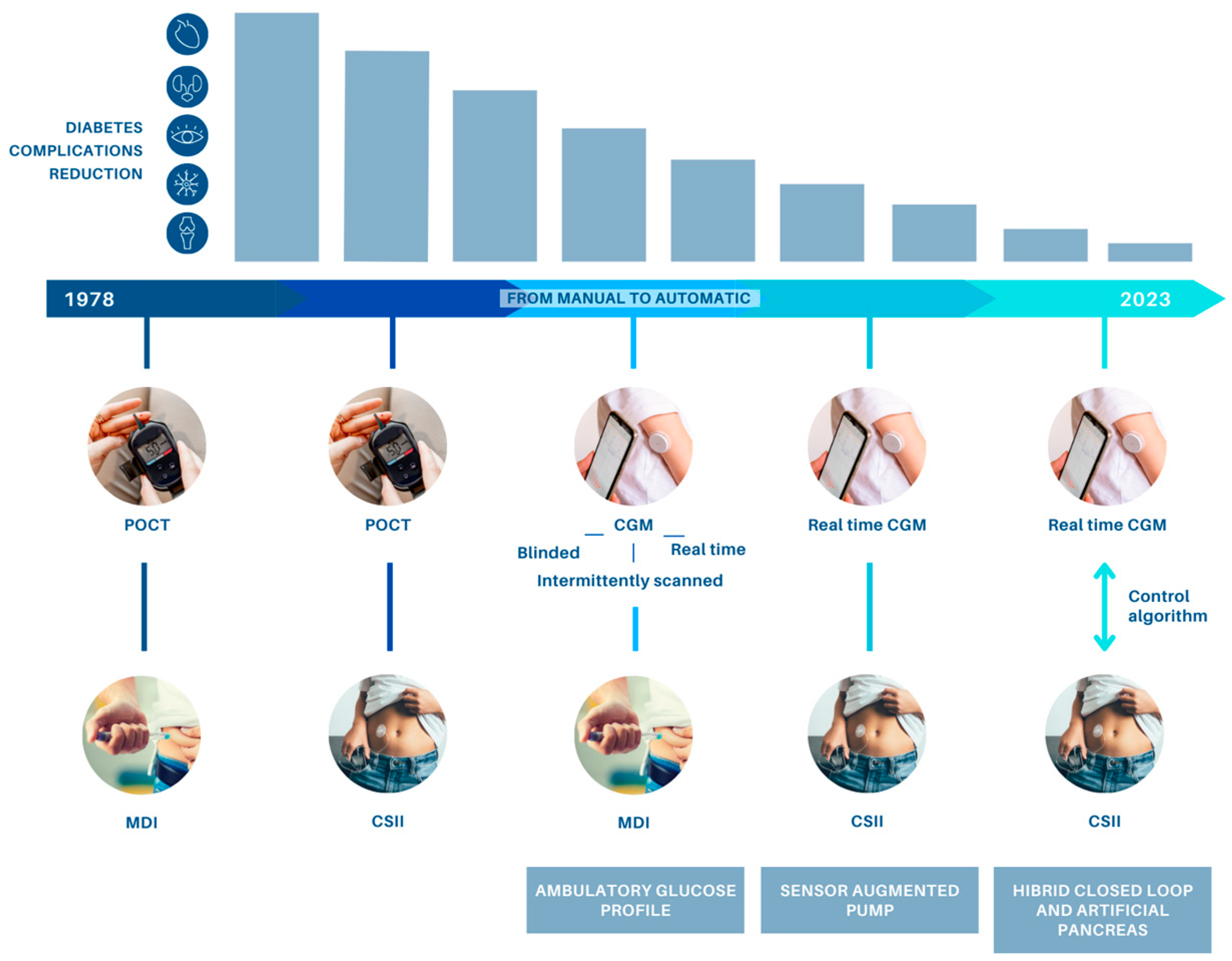
6. Insulin Pump Without Needles? (Patch-Based Delivery)
Some companies are developing needle-free insulin pumps that use alternative methods to deliver insulin through the skin.
Examples include:
Jet injection technology:
Uses high-pressure streams of insulin to penetrate the skin without a needle.
Ultrasound-assisted delivery:
Uses sound waves to temporarily open pathways in the skin, allowing insulin to pass through.
Electric field-based delivery (electroporation):
Uses mild electrical pulses to increase skin permeability to insulin.
These methods are still largely experimental but show promise for pediatric use.
Beyond Insulin: Alternative Approaches to Treating Diabetes in Children
Instead of just changing how insulin is delivered, some global projects aim to treat the root cause of type 1 diabetes.
7. Islet Cell Transplantation (Biological Cure Attempts)
In type 1 diabetes, the body’s immune system destroys insulin-producing beta cells in the pancreas. Researchers are trying to replace these cells.
How it works:
Healthy insulin-producing cells are transplanted into the patient’s body.
These cells begin producing insulin naturally.
Global efforts:
Canada (Edmonton Protocol):
One of the most successful early approaches to islet transplantation.
USA and Europe:
Trials are ongoing using encapsulated islet cells (protected from the immune system without strong immunosuppressive drugs).
For children:
This approach could potentially eliminate the need for insulin entirely. However:
It is complex
It is expensive
It is not yet widely available
It still carries medical risks
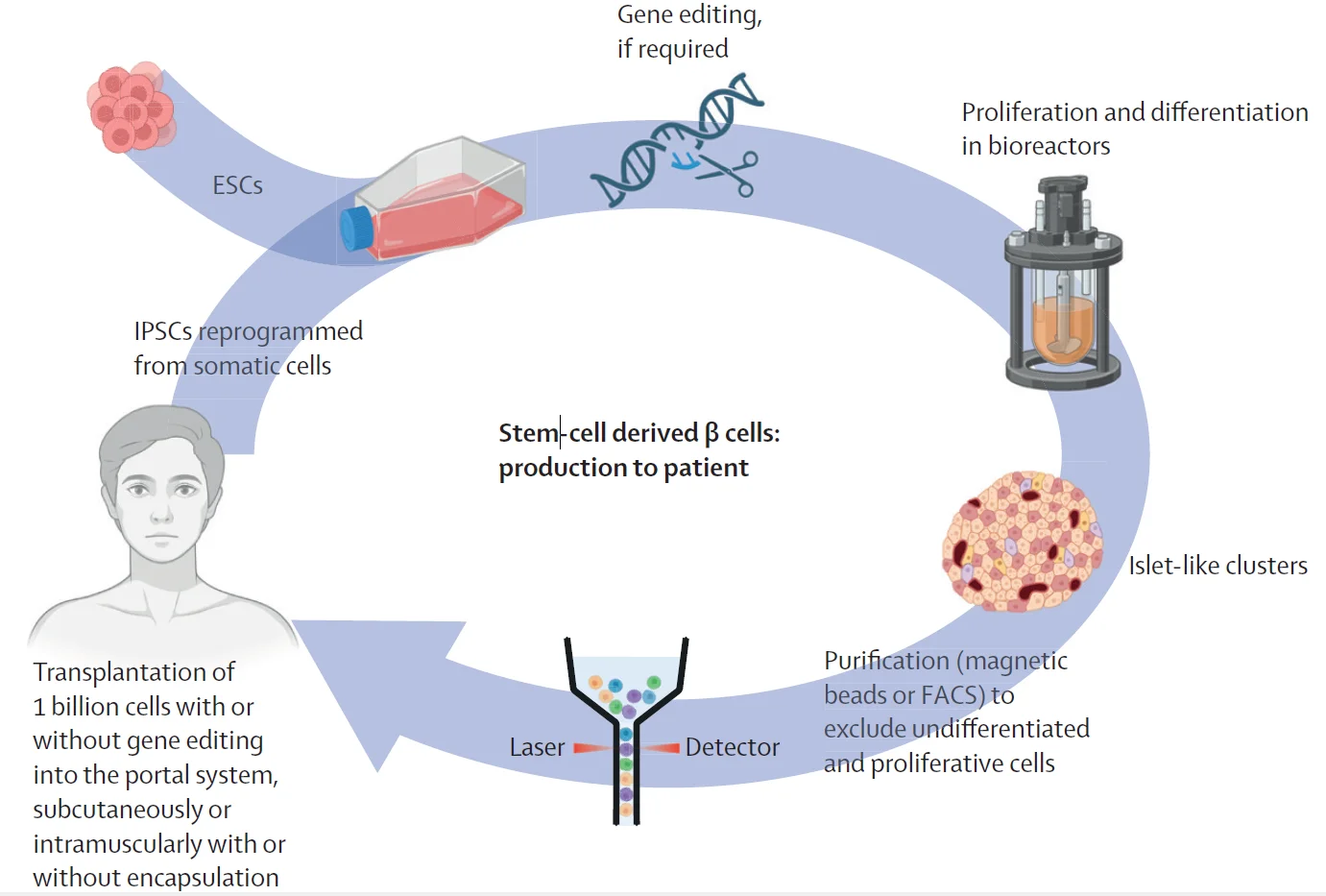
8. Stem Cell Therapy
Stem cells are immature cells that can develop into different types of cells, including insulin-producing beta cells.
Global research:
USA (ViaCyte, Vertex Pharmaceuticals):
Developing stem-cell-derived beta cells that can be implanted into the body.
Europe and Japan:
Similar projects are underway to create functional insulin-producing cells in the lab.
Potential future:
If successful, this could be a near-cure for type 1 diabetes, meaning children might no longer need insulin injections at all.
Artificial Pancreas Without Needles?
Even current artificial pancreas systems still require:
A CGM sensor inserted under the skin
An insulin pump catheter under the skin
However, future versions may combine:
Non-invasive glucose monitoring (through skin or wearable devices)
Needle-free insulin delivery methods
This could eventually create a completely needle-free artificial pancreas.
Barriers to Needle-Free Treatment
Despite exciting progress, several major challenges remain:
1. Scientific Challenges
Getting insulin into the body effectively without needles is extremely difficult.
Insulin must be absorbed quickly and predictably.
Variability between individuals makes standardization hard.
2. Safety Concerns in Children
Children are still growing, so:
Long-term effects must be carefully studied
Lungs, skin, and immune systems may react differently than adults
3. Regulatory Approval
New technologies must pass rigorous clinical trials before being approved for children, which can take many years.
4. Cost and Access
Even if needle-free treatments become available, they may initially be:
Very expensive
Available only in high-income countries
This raises concerns about global health inequality.
What Is Realistic in the Next 5–10 Years?
Based on current research trends, experts predict:
In 5 years:
More advanced insulin pumps and CGMs
Better AI-driven closed-loop systems
Possibly limited use of inhalable insulin in some children
In 10 years:
More widespread use of smart insulin
Improved microneedle patches
More progress in stem cell and islet transplantation
In 15–20 years:
Possible functional cures for some children
Fully automated, possibly needle-free artificial pancreas systems
Final Conclusion: Is a Needle-Free Future on the Way?
Yes — but gradually, not overnight.
We are not there yet, but the world is clearly moving toward:
Fewer injections
Less invasive treatment
More automated and biological solutions
For children with diabetes, the future looks significantly brighter than the past.
Right now, treatment is becoming:
Safer
Easier
Less painful
More child-friendly
In the coming decades, it is very possible that many children diagnosed with type 1 diabetes will grow up with little or no need for daily injections.
Is the Treatment of Children’s Diabetes Without Injections on the Way? — Final Expansion
What Do Children and Parents Actually Want? (Patient-Centered Perspective)
While scientists focus on technology and biology, it is crucial to listen to the voices of children with diabetes and their families.
Children’s priorities
When surveyed globally, many children with type 1 diabetes express that they want:
1. Less pain and fewer needles
The fear of injections can be intense, especially in younger children.
Needle anxiety can sometimes be worse than the disease itself.
2. More freedom
Being able to play, travel, and attend school without constant medical routines.
3. Less visibility of diabetes
Many children feel embarrassed about injecting insulin in public or wearing visible devices.
Parents’ priorities
Parents often emphasize:
1. Safety above all
Preventing severe hypoglycemia (dangerously low blood sugar), especially at night.
2. Reliability
Any new needle-free system must be predictable and trustworthy.
3. Simplicity
Treatments that reduce complexity, not add more technology to manage.
These perspectives strongly shape research priorities worldwide.
How Governments and Health Systems Are Responding
Several countries are actively investing in needle-free or less invasive diabetes technologies.
United States
Major funding from:
National Institutes of Health (NIH)
JDRF (Juvenile Diabetes Research Foundation)
Strong support for:
Artificial pancreas systems
Stem cell research
Smart insulin development
European Union
Large collaborative research projects involving multiple countries.
Focus on:
Microneedle patches
Non-invasive glucose monitoring
Encapsulated islet cell transplantation
Japan and South Korea
Leaders in:
Wearable medical devices
Miniaturized technology
Advanced biomaterials for drug delivery
India and China
Significant work on:
Oral insulin formulations
Low-cost technologies for broader accessibility
This global effort suggests that needle-free treatment is not just a dream, but a coordinated international mission.
Economic Implications: Will Needle-Free Treatment Be Affordable?
A major question is whether these new technologies will be accessible to all children.
Initial Costs
New treatments are likely to be:
Expensive at first
Available mainly in high-income countries
Examples:
Early artificial pancreas systems were initially very costly.
Stem cell therapies, if approved, may be extremely expensive.
Long-Term Savings
However, needle-free or near-curative treatments could:
Reduce hospitalizations
Prevent long-term complications
Decrease emergency care costs
Reduce burden on families and healthcare systems
Over time, this could actually make them economically beneficial.
Ethical Questions About a Needle-Free Future
Scientific progress also raises important ethical issues.
1. Who gets access first?
If a breakthrough needle-free treatment becomes available, who should receive it first?
Wealthy families?
Children with the most severe diabetes?
Those with poorest access to current care?
These are difficult moral questions.
2. Human vs. Technological Care
If AI and automated systems take over most diabetes management, will children lose important self-care skills?
Experts argue that education should always remain part of treatment, even with advanced technology.
3. Data and Privacy
Many modern diabetes technologies collect large amounts of personal health data.
Questions include:
Who owns this data?
How is it stored?
Can insurance companies access it?
Strong privacy protections will be essential.
Scientific Roadmap: What Needs to Happen Next?
To make needle-free diabetes treatment a reality, researchers must solve several key problems:
Step 1: Better Insulin Delivery
Improve absorption through skin, lungs, or gut.
Make dosing more predictable and consistent.
Step 2: Safer Long-Term Use
Conduct large pediatric clinical trials.
Ensure no harmful effects on growth, development, or organs.
Step 3: Integration with AI
Combine needle-free insulin with smart algorithms.
Create fully automated systems that need minimal human input.
Step 4: Global Accessibility
Reduce manufacturing costs.
Make technologies available in low- and middle-income countries.
Most Likely Scenario: Gradual Transformation, Not Sudden Cure
Based on current science, the future will probably unfold like this:
Short term (5 years)
Fewer injections, not zero.
More use of:
Microneedle patches
Better insulin pumps
Smarter AI-driven systems
Medium term (10–15 years)
Possible widespread use of:
Smart insulin
Advanced oral insulin in some cases
More successful islet or stem cell therapies
Long term (20+ years)
Potential functional cures for some children.
Completely needle-free or nearly needle-free diabetes management for many.
Final Conclusion: Are We Close?
Yes — but cautiously.
We are not yet at a point where all children with diabetes can live completely without injections.
However, the direction of global research is clear:
Less invasive
More automated
More biological
More child-friendly
The question is no longer if needle-free treatment will arrive — but when, for whom, and in what form.
For today’s children with diabetes, treatment is already far better than it was 10–20 years ago. For tomorrow’s children, it may look completely different.