Insulin Pump + CGM + Artificial Intelligence: The Automatic Treatment of Children’s Diabetes
Introduction: A New Era in Pediatric Diabetes Care
Type 1 diabetes in children requires constant and precise management. Unlike adults, children experience rapid changes in blood sugar due to growth, hormones, unpredictable eating habits, physical activity, stress, and sleep patterns.
Traditionally, this meant frequent finger-prick glucose checks, multiple daily insulin injections, careful meal planning, and continuous parental vigilance—often leading to stress, anxiety, and sleep deprivation for families.
In the last decade, a powerful technological transformation has occurred in pediatric diabetes care through the integration of three key components:
1. Insulin Pump
2. Continuous Glucose Monitor (CGM)
3. Artificial Intelligence (AI)-driven algorithms
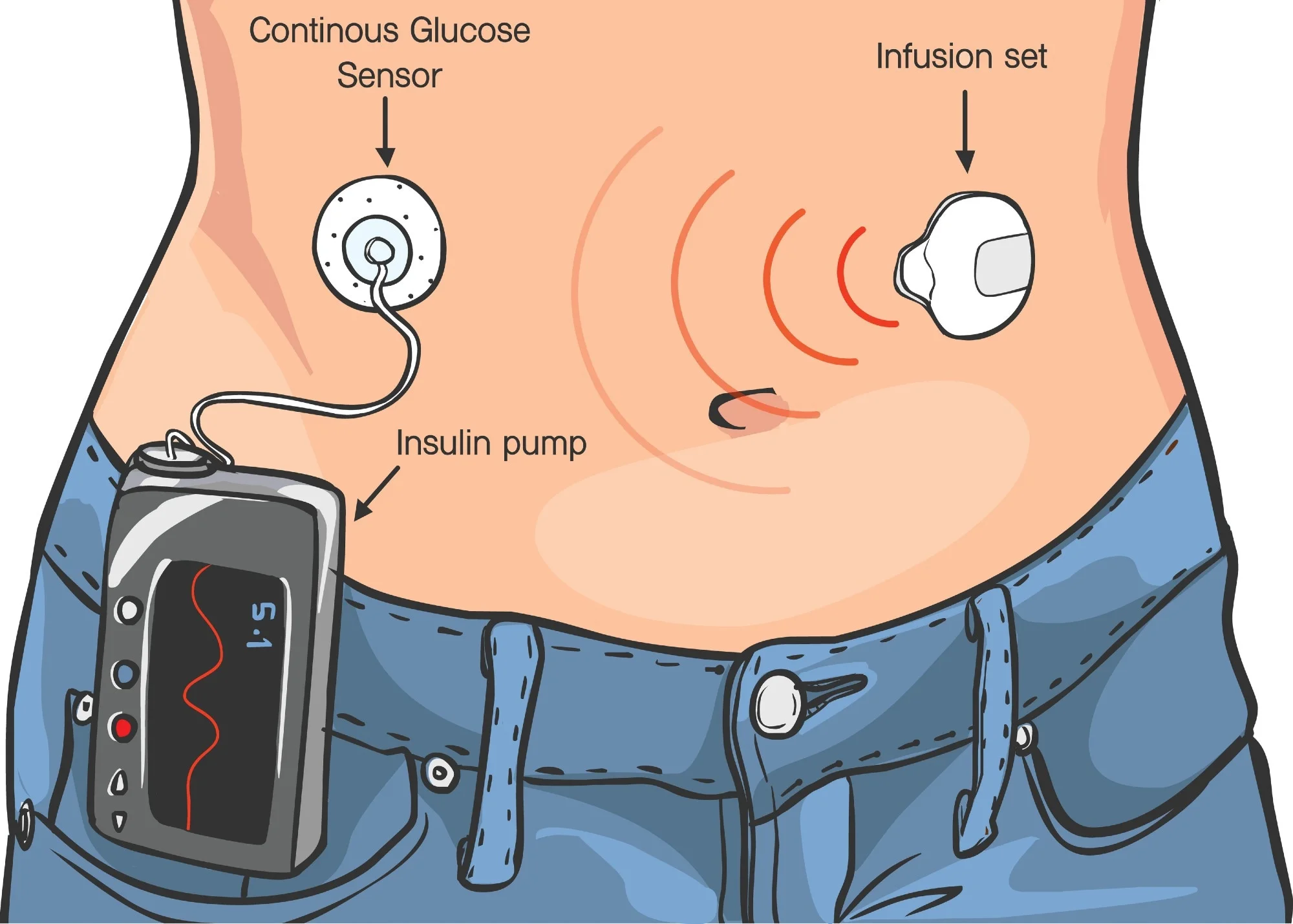
Together, these form an automated insulin delivery system, often called a closed-loop system or artificial pancreas. This combination represents one of the most significant medical revolutions in the treatment of childhood diabetes.
Understanding the Three Core Components
1. The Insulin Pump: Smart Insulin Delivery
An insulin pump is a small wearable device that continuously delivers rapid-acting insulin through a tiny catheter placed under the skin. Unlike traditional injections, which provide insulin in fixed doses at specific times, the pump can:
Deliver basal insulin (small amounts continuously throughout the day and night)
Provide bolus doses (extra insulin for meals)
Adjust insulin delivery based on activity, illness, or other factors
For children, this means:
No more multiple daily injections
More flexibility in eating and activity
More precise insulin dosing
However, on its own, an insulin pump still requires manual decisions by parents or the child—this is where CGM and AI come into play.
2. Continuous Glucose Monitor (CGM): Real-Time Blood Sugar Awareness
A CGM is a small sensor inserted under the skin that measures glucose levels in the interstitial fluid every few minutes. It wirelessly sends this data to a receiver, smartphone, or insulin pump.
Key advantages of CGM include:
Continuous monitoring instead of occasional finger pricks
Trend arrows showing whether glucose is rising or falling
Alarms for high or low blood sugar
Nighttime monitoring without waking the child
For parents, CGM provides peace of mind. Instead of guessing what is happening inside their child’s body, they can see real-time glucose patterns.
But even with a pump and CGM, someone still needs to interpret the data and adjust insulin. This is where Artificial Intelligence becomes transformative.
3. Artificial Intelligence: The Brain of the System
Artificial Intelligence (AI) in diabetes care refers to advanced computer algorithms that analyze glucose data in real time and make automatic insulin delivery decisions.
Instead of humans constantly calculating insulin doses, the AI system does the following:
1. Reads glucose levels from the CGM every few minutes
2. Predicts where blood sugar is heading
3. Adjusts insulin delivery through the pump accordingly
This creates a closed-loop system, meaning:
1. The system measures glucose
2. The AI decides how much insulin is needed
3. The pump delivers the insulin automatically
This process happens continuously, day and night, without constant human intervention.
How This Works in Real Life for a Child
Imagine a typical day for a child using this system:
Morning
The child wakes up.
During the night, the AI system has already adjusted insulin to prevent both high and low blood sugar.
The child starts the day with stable glucose levels.
Breakfast
The child eats.
In most current systems, parents still announce the meal and estimate carbohydrates.
The AI fine-tunes insulin delivery based on real-time glucose response.
School Time
The child plays, runs, or participates in sports.
Instead of manually reducing insulin beforehand, the AI detects falling glucose levels and automatically decreases insulin delivery.
Nighttime
While the child sleeps, the system continues to monitor and adjust insulin.
If blood sugar starts dropping, insulin delivery is reduced or stopped.
If blood sugar rises, insulin is increased.
For many families, this has dramatically reduced nighttime anxiety and improved sleep quality.
Why AI Makes This Truly ‘Automatic’
Traditional diabetes management depends heavily on human decision-making, which can be:
Emotionally exhausting
Prone to error
Difficult during sleep or illness
AI changes this by:
Learning from past glucose patterns
Adapting to each child’s unique metabolism
Responding faster than humans to sudden glucose changes
Reducing the risk of both high and low blood sugar
In essence, AI acts like a highly intelligent, always-awake diabetes assistant.

Benefits of AI-Driven Insulin Pump + CGM Systems in Children
1. Better Blood Sugar Control
Studies show that children using AI-driven closed-loop systems spend significantly more time within the target glucose range (70–180 mg/dL). This leads to:
Fewer dangerous highs and lows
More stable energy levels
Better overall health outcomes
2. Reduced Risk of Hypoglycemia (Low Blood Sugar)
Hypoglycemia is one of the most feared complications of diabetes, especially at night. AI systems are particularly good at preventing this by:
Detecting downward trends early
Automatically reducing insulin delivery
Preventing severe drops before they happen
3. Less Burden on Parents and Caregivers
Before this technology, parents often had to:
Wake up multiple times per night
Constantly monitor glucose levels
Calculate insulin doses manually
Now, much of this work is handled automatically, leading to:
Less stress
Better sleep
Improved family well-being
4. More Freedom for Children
Children can:
Play sports more freely
Attend school without constant interruptions
Feel less “different” from their peers
Many children report feeling more independent and confident.
Current Limitations and Challenges
Despite its many advantages, the system is not perfect.
Not Fully Hands-Off Yet
Most current systems are “hybrid” closed-loop, meaning:
They still require meal announcements
Parents must estimate carbohydrates
The system cannot yet fully handle every situation automatically
Cost and Accessibility
These systems are expensive, and access varies by country. Not all families can afford them or get insurance coverage.
Technical Issues
Occasionally, sensors fail, pumps malfunction, or connectivity problems occur, requiring human intervention.
Need for Education
Families still need training to understand how the system works and how to respond when something goes wrong.
The Future: Toward Fully Automated Diabetes Care
Researchers are actively developing next-generation systems that aim to be:
Fully automated (no meal announcements needed)
More accurate in predicting glucose changes
Smaller, more comfortable, and less visible
Capable of delivering both insulin and glucagon (dual-hormone systems)
In the future, children with diabetes may only need to wear a small device that quietly and automatically manages their blood sugar with minimal effort from them or their parents.
Long-Term Impact on Children’s Health
Better glucose control from an early age could significantly reduce the risk of long-term complications such as:
Eye damage (retinopathy)
Kidney disease (nephropathy)
Nerve damage (neuropathy)
Cardiovascular problems
This means that today’s children using AI-driven systems may grow into healthier adults compared to previous generations with diabetes.
Conclusion: A True Revolution in Pediatric Diabetes Treatment
The combination of insulin pump + CGM + artificial intelligence represents a real transformation in the treatment of childhood diabetes.
It moves diabetes care from:
Manual → Automated
Reactive → Predictive
Stressful → More manageable
While it does not cure diabetes, it is the closest we have ever come to replicating the natural function of the human pancreas.
For children, this means:
Safer blood sugar
More freedom
A more normal childhood
For parents, it means:
Less fear
Better sleep
Greater peace of mind
And for medicine, it marks the beginning of a new era where intelligent technology works hand-in-hand with the human body to improve lives.
Real-World Use: What Actually Happens in Daily Life
While clinical studies show impressive numbers, the true meaning of this technology becomes clear in everyday life.
A Typical Family Before vs. After AI Automation
Before (traditional treatment):
Parents wake up several times at night to check blood sugar.
The child often experiences highs after meals and lows during play.
School nurses must be heavily involved.
Parents constantly worry about emergencies.
Family routines revolve around diabetes management.
After (Insulin Pump + CGM + AI):
The system adjusts insulin automatically through the night.
Parents sleep more peacefully.
The child can play sports with fewer interruptions.
Blood sugar fluctuations are smoother and less extreme.
Diabetes becomes less visible and less dominant in family life.
Many families describe this transition as “getting their life back.”
How AI Actually ‘Learns’ the Child’s Body
The AI in these systems is not generic—it gradually adapts to each child’s unique physiology.
It takes into account:
How sensitive the child is to insulin
Typical glucose patterns during sleep
Responses to different meals
Effects of physical activity
Hormonal changes (especially during puberty)
Over time, the system becomes better at predicting how the child’s glucose will behave in different situations. This personalization is one of the greatest strengths of AI-driven diabetes care.
Clinical Impact: What Doctors Are Seeing
Pediatric endocrinologists around the world are observing major changes in their practice.
More Stable Patients
Doctors report:
Fewer extreme glucose swings
Better overall glucose control (HbA1c and time-in-range)
Fewer emergency visits for hypoglycemia or diabetic ketoacidosis
Shift in Medical Focus
Instead of spending most of clinic time adjusting insulin doses, doctors now focus more on:
Growth and development
Nutrition and lifestyle
Psychological well-being
Supporting families emotionally
This represents a more holistic approach to diabetes care.
Psychological Effects on Children and Adolescents
Reduced Anxiety and Fear
Many children previously lived in fear of:
Low blood sugar episodes
Embarrassment at school
Being “different” from friends
With automated systems, children often feel:
Safer
More confident
Less controlled by their disease
Greater Independence
Older children and teenagers can gradually take more responsibility for their diabetes without being overwhelmed. AI acts as a safety net, allowing them to be more independent while still protected.
Improved Quality of Childhood
Instead of constantly thinking about diabetes, many children can simply focus on being children—playing, learning, and growing.
Challenges That Families Still Face
Despite major progress, this technology does not eliminate all difficulties.
1. Wearing Devices
Children must wear:
A CGM sensor
An insulin pump or pod
Some children may feel uncomfortable or self-conscious about this, especially in adolescence.
2. Alarms and Alerts
Although AI reduces many alarms, occasional alerts still occur, which can be annoying or disruptive.
3. Technical Dependence
Families must still be prepared for:
Sensor failures
Pump malfunctions
Battery issues
This means traditional diabetes knowledge remains important.
Ethical and Social Considerations
Technology vs. Human Care
Some critics worry that heavy reliance on AI might reduce:
Parents’ understanding of diabetes
Children’s ability to self-manage in emergencies
For this reason, education and backup plans remain essential.
Health Inequality
One of the biggest ethical issues is that:
Wealthier families and countries have better access to this technology
Many children worldwide still lack basic insulin and glucose monitoring
This raises important questions about fairness in global health.
Economic Impact: Is It Worth the Cost?
These systems are expensive, but they may be cost-effective in the long run.
Potential savings include:
Fewer hospitalizations
Reduced emergency room visits
Lower risk of long-term complications
Less time parents miss from work
Many health economists believe that widespread adoption could ultimately reduce the overall financial burden of diabetes on healthcare systems.
Comparison: Human vs. AI Decision-Making in Diabetes
| Situation | Human Decision | AI System Response |
|---|---|---|
| Rising glucose after meals | May react slowly | Adjusts insulin in real time |
| Falling glucose during sleep | May go unnoticed | Automatically reduces insulin |
| Exercise-induced lows | Requires planning | Detects trends and adapts |
| Illness or stress | Hard to predict | Gradually adapts based on data |
| Day-to-day variability | Prone to error | More consistent |
This table illustrates why AI has become such a powerful tool in pediatric diabetes management.
Current Systems vs. Future Systems
Today: Hybrid Closed-Loop
Most systems today still require:
Meal announcements
Carb counting
Some level of human involvement
Tomorrow: Fully Automated Systems
Researchers aim to create systems that:
Do not require meal input
Automatically detect eating based on glucose patterns
Use faster-acting insulin
Possibly deliver both insulin and glucagon
This could bring us even closer to a true “bionic pancreas.”
What This Means for the Next Generation of Children with Diabetes
Children diagnosed with type 1 diabetes today are growing up in a very different era than previous generations.
Compared to the past, they are more likely to:
Have stable blood sugar
Avoid severe complications
Live with less fear and stress
Experience a more normal childhood
Many experts believe that this technology will shape a healthier, more confident generation of young people with diabetes.
Final Conclusion: From Burden to Balance
The combination of Insulin Pump + CGM + Artificial Intelligence represents a fundamental transformation in how childhood diabetes is treated.
It shifts diabetes care from:
Constant human effort → Intelligent automation
Crisis management → Continuous prevention
Fear and stress → Safety and stability
Although it does not cure diabetes, it dramatically changes what it means to live with the disease.
For children, this system offers:
Better health
More freedom
A brighter future
For families, it offers:
Peace of mind
Better sleep
Less emotional burden
And for medicine, it represents a powerful example of how technology and human care can work together to improve lives.