Managing Type 1 Diabetes in children—especially those with active, energetic lifestyles—requires careful selection of insulin delivery methods.
Insulin pumps are a widely used option and come in two main types: tubed pumps and tubeless (patch) pumps.
Each has distinct advantages and limitations, particularly when it comes to children who are frequently moving, playing, or participating in sports.
This article provides a comprehensive comparison to help parents and caregivers make informed decisions.
1. Basic Design and Function
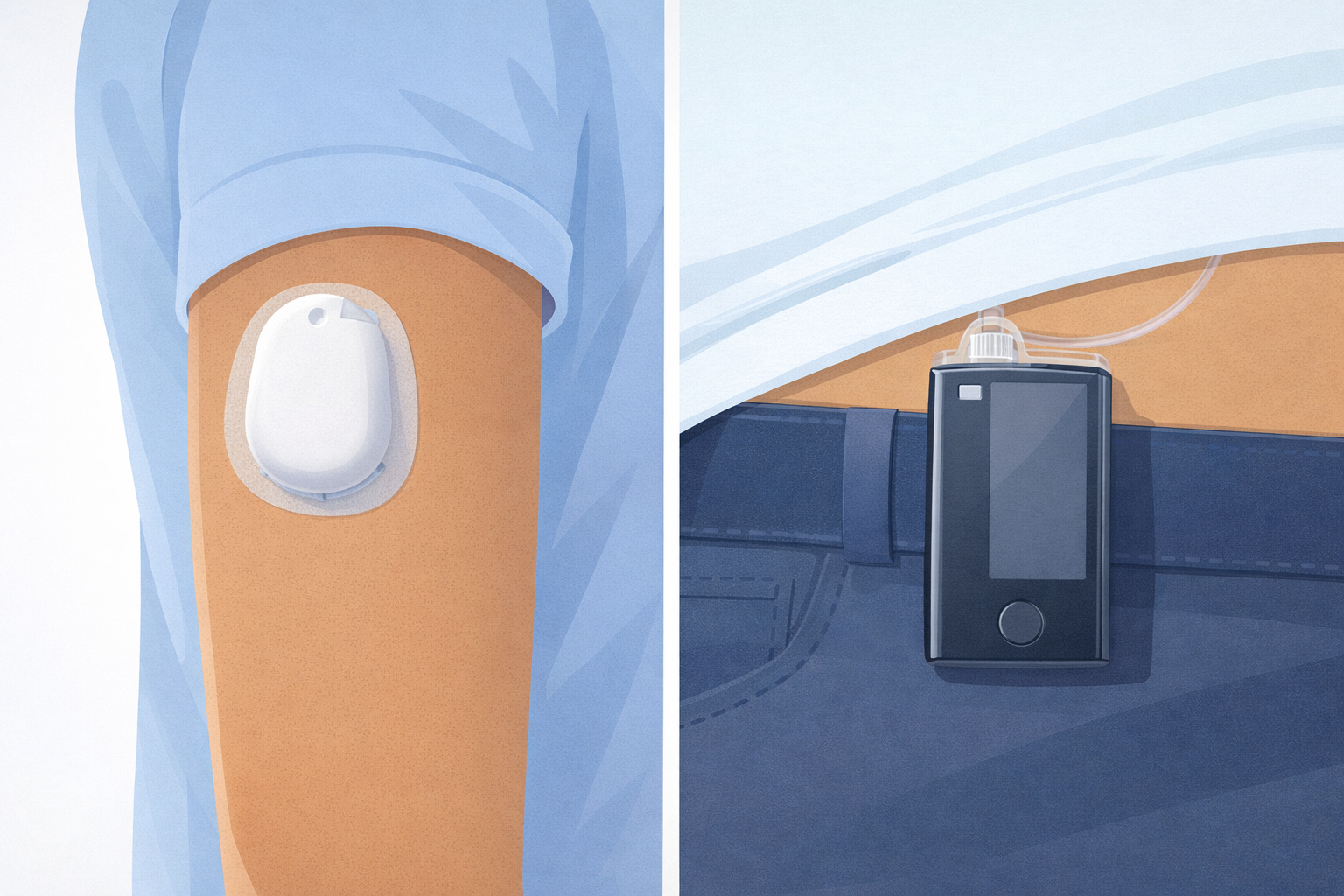
Tubed insulin pumps deliver insulin through a thin plastic tube connected to a cannula inserted under the skin. The pump itself is a separate device that can be clipped to clothing or carried in a pocket.
Tubeless pumps (patch pumps) are self-contained units that adhere directly to the skin. They deliver insulin without any external tubing and are typically controlled via a remote device or smartphone app.
2. Freedom of Movement and Physical Activity
For active children, mobility and comfort during movement are critical.
Tubeless Pumps:
These are often preferred for sports and high-energy play because there is no tubing to snag or pull. This reduces the risk of accidental dislodging during activities like running, climbing, or contact sports.
Tubed Pumps:
The tubing can sometimes get caught on objects or pulled during rough play. While many children adapt to this, it may require extra precautions (e.g., securing the tubing or temporarily disconnecting during intense activity).
3. Comfort and Ease of Use
Tubeless Pumps:
Many children find these more comfortable and less intrusive since they are compact and worn directly on the skin. There is no separate device to carry around.
Tubed Pumps:
Some children may feel bothered by having both a device and tubing. However, others quickly get used to wearing it and may not find it problematic over time.
4. Insulin Delivery Control and Features
Both pump types allow for programmable basal rates and bolus dosing.
Tubed Pumps:
Often offer more advanced customization options and fine-tuned control. They may be preferred in cases where highly precise insulin adjustments are needed.
Tubeless Pumps:
Typically controlled via a handheld device or app, which can be convenient for parents monitoring younger children. However, some models may have fewer advanced features compared to high-end tubed pumps.
5. Durability and Risk of Dislodgement
Tubeless Pumps:
Being directly attached to the skin reduces the number of external components. However, if the device is knocked off, the entire unit must be replaced.
Tubed Pumps:
If something goes wrong, often only the infusion set or tubing needs to be replaced rather than the entire system. On the downside, more components mean more potential points of failure.
6. Use During Water Activities
Tubeless Pumps:
Many models are waterproof, allowing children to swim or bathe without removing the device.
Tubed Pumps:
Some need to be disconnected during swimming or showering, which may temporarily interrupt insulin delivery.
7. Cost Considerations
Tubeless Pumps:
Usually involve higher ongoing costs because the entire patch unit is replaced every few days.
Tubed Pumps:
May be more cost-effective long term since only the infusion set and reservoir are replaced regularly.
8. Social and Psychological Impact
Children often want to feel “normal” among their peers.
Tubeless Pumps:
These are more discreet and less noticeable, which can boost confidence and reduce self-consciousness.
Tubed Pumps:
More visible and may attract attention, though many children become comfortable with them over time.
9. Parental Monitoring and Safety
Tubeless Pumps:
Remote control features can allow parents to monitor and adjust insulin delivery without interrupting the child’s activity.
Tubed Pumps:
Some models also integrate with continuous glucose monitoring systems, offering strong safety features, though direct remote control may vary.
Conclusion
There is no one-size-fits-all solution when choosing between tubed and tubeless insulin pumps for active children.
Choose tubeless pumps if your priority is freedom of movement, ease of wear, and minimal interference with physical activity.
Choose tubed pumps if you value advanced control, flexibility in components, and potentially lower long-term costs.
Ultimately, the best choice depends on the child’s activity level, preferences, medical needs, and family lifestyle. Consulting with a healthcare provider is essential to ensure optimal management of diabetes and long-term well-being.
10. Integration with Continuous Glucose Monitoring (CGM)
Modern diabetes care increasingly relies on combining insulin pumps with continuous glucose monitoring systems.
Tubed Pumps:
Many advanced tubed pumps integrate seamlessly with CGMs to form hybrid closed-loop systems (sometimes called “artificial pancreas” systems). These systems can automatically adjust insulin delivery based on glucose readings, which is particularly helpful for active children whose glucose levels fluctuate rapidly during exercise.
Tubeless Pumps:
Some tubeless options also integrate with CGMs and offer automated insulin delivery. While historically slightly behind in integration features, newer models are quickly catching up and now provide competitive automation capabilities.
For children with unpredictable activity patterns, this integration can significantly reduce the burden of manual adjustments and improve overall glucose control.
11. Site Rotation and Skin Health
Proper rotation of infusion sites is essential to avoid skin irritation, lipohypertrophy, and inconsistent insulin absorption.
Tubeless Pumps:
Because the entire device adheres to the skin, it requires sufficient surface area for placement. Rotating sites (arms, abdomen, thighs, lower back) is crucial, but some children may find fewer comfortable locations due to the size of the patch.
Tubed Pumps:
The infusion set is typically smaller, offering more flexibility in placement. This can make site rotation easier, especially for lean or younger children.
Children with sensitive skin may need to experiment with adhesives, barrier wipes, or protective patches regardless of pump type.
12. Learning Curve and Training
Starting insulin pump therapy involves education for both the child and caregivers.
Tubed Pumps:
These may require a slightly steeper learning curve due to multiple components (pump, tubing, infusion set). However, they often provide detailed feedback and settings that can help families fine-tune therapy over time.
Tubeless Pumps:
Generally simpler in design, which can make initial training easier. The all-in-one format reduces the number of steps required for setup and daily use.
For very young children or busy families, simplicity can be a major advantage.
13. Battery, Charging, and Technical Reliability
Tubeless Pumps:
Typically use built-in batteries that last for the lifespan of the patch (usually 2–3 days). Once depleted, the entire unit is replaced.
Tubed Pumps:
Use rechargeable or replaceable batteries. While this adds one more element to manage, it also allows longer device use without full replacement.
From a reliability standpoint, both systems are generally robust, but families should always have backup insulin delivery methods available in case of technical issues.
14. Suitability by Age Group
Toddlers and Young Children:
Tubeless pumps are often preferred due to fewer detachable parts and reduced risk of pulling on tubing.
School-Age Children:
Either option can work well. The choice often depends on the child’s activity level and willingness to manage the device.
Adolescents:
Teenagers may prioritize discretion and appearance, making tubeless pumps appealing. However, those interested in fine-tuning control (e.g., athletes) may prefer advanced tubed systems.
15. Sports-Specific Considerations
Different sports present different challenges:
Contact Sports (e.g., football, martial arts):
Tubeless pumps reduce snagging risk, but protective padding may still be needed.
Water Sports (e.g., swimming):
Waterproof tubeless pumps provide continuous insulin delivery, whereas tubed pumps may need removal.
Endurance Activities (e.g., running, cycling):
Both systems can work well, but integration with CGM and automated insulin adjustment becomes especially valuable.
16. Real-Life Adaptability
No matter how advanced a pump is, real-life usability matters most.
Children may forget to reconnect tubed pumps after removing them.
Tubeless pumps may occasionally fall off due to sweat or friction.
Growth, hormonal changes, and daily routines will all influence which system works best over time.
Flexibility and willingness to reassess the choice periodically are key.
Final Thoughts
Choosing between tubed and tubeless insulin pumps is not just a technical decision—it’s a lifestyle decision. For children living with Type 1 Diabetes, the goal is to enable safe, effective insulin delivery while preserving freedom, confidence, and joy in daily activities.
Both systems have evolved significantly and can support excellent diabetes management. The “best” option is the one that:
Fits naturally into the child’s daily life
Minimizes disruptions during play and school
Provides reliable glucose control
Is comfortable and acceptable to the child
Families should work closely with healthcare providers, and whenever possible, involve the child in the decision-making process. Empowerment and comfort often lead to better long-term adherence and outcomes in managing diabetes.

17. Alarms, Alerts, and Safety Features
Safety is a central concern for children with Type 1 Diabetes, especially during school, sleep, and sports.
Tubed Pumps:
Typically offer a wide range of alarms—occlusion alerts (blockages), low reservoir warnings, battery alerts, and reminders for missed boluses. When paired with CGM systems, they may also provide predictive alerts for rising or falling glucose levels.
Tubeless Pumps:
Also include essential alarms, though the way alerts are delivered often depends on the external controller or smartphone. Some systems rely heavily on the controller being nearby, which can be a limitation if the child leaves it behind.
For active children who may not always pay attention to subtle alerts, louder and more customizable alarm systems can be particularly valuable.
18. Nighttime Management and Sleep Quality
Managing glucose levels overnight is one of the biggest challenges for families.
Tubed Pumps:
When integrated with CGM, many models can automatically adjust basal insulin overnight, reducing the risk of hypoglycemia. However, tubing can occasionally become tangled during sleep, especially in restless sleepers.
Tubeless Pumps:
Offer a more streamlined experience during sleep with no tubing to worry about. This can improve comfort and reduce the likelihood of accidental dislodging at night.
Parents often report better peace of mind when automation features are combined with reliable overnight alerts.
19. School Environment and Independence
Children spend a large portion of their day at school, making ease of use in that setting crucial.
Tubeless Pumps:
Allow discreet insulin dosing via a handheld device, meaning the child does not need to expose the pump in public. This can reduce stigma and make it easier to manage diabetes without drawing attention.
Tubed Pumps:
May require accessing the pump physically, which can be slightly less discreet depending on how it is worn. However, some children and school staff appreciate the tactile, always-available interface.
For younger children, teachers and school nurses may need training regardless of the pump type.
20. Travel and Daily Logistics
Active families often travel, whether for vacations, sports competitions, or daily commuting.
Tubeless Pumps:
Require carrying multiple disposable pods for replacement every few days. While convenient in use, forgetting supplies can be problematic.
Tubed Pumps:
Require infusion sets, reservoirs, and possibly extra batteries or charging equipment. There are more components to manage, but also more flexibility if one part fails.
Both systems require careful planning, including backup insulin (such as pens or syringes).
21. Data Tracking and Digital Ecosystem
Modern diabetes devices often include apps and cloud-based data sharing.
Tubed Pumps:
Many systems offer detailed data analytics, trend reports, and integration with healthcare platforms. This can help parents and clinicians make informed adjustments.
Tubeless Pumps:
Increasingly offer strong app ecosystems, allowing remote monitoring and easier data sharing. Some are particularly user-friendly for families who prefer smartphone-based management.
Data visibility is especially important for active children, as physical activity can cause rapid and unpredictable glucose changes.
22. Emotional Well-being and Long-Term Adherence
Beyond physical function, emotional acceptance of the device plays a major role in long-term success.
Tubeless Pumps:
Often feel less “medical” and more like a wearable gadget, which can improve acceptance—especially in younger children or those sensitive to body image.
Tubed Pumps:
May initially feel more intrusive, but some children grow to appreciate the control and reliability they offer.
A child who feels comfortable and confident with their device is more likely to use it consistently and correctly.
23. When to Reconsider Your Choice
It’s important to recognize that the “right” pump today may not be the best choice in the future.
You may want to reassess if:
The child’s activity level changes significantly
There are frequent technical issues or discomfort
Glucose control is not meeting targets
The child expresses frustration or resistance
New technologies become available
Diabetes management is dynamic, and flexibility is key to long-term success.
Comprehensive Summary
For active children living with diabetes, both tubed and tubeless insulin pumps offer powerful tools for maintaining glucose control while supporting a full, active life.
Tubeless Pumps – Key Strengths:
Greater freedom of movement
No tubing to manage
More discreet and often more comfortable
Better suited for sports and water activities
Tubed Pumps – Key Strengths:
Advanced control and customization
Often more detailed data and integration
Lower long-term consumable costs
Flexible component replacement
Final Perspective
The decision ultimately comes down to balancing medical needs, lifestyle demands, and personal preferences.
An active child should not feel limited by their diabetes management tools. The ideal pump is one that becomes a seamless part of their life—supporting them during sports, school, sleep, and play without constant disruption.
Close collaboration with healthcare providers, ongoing education, and open communication with the child will ensure the chosen system continues to meet evolving needs.

